Table of Contents
ToggleCut Time, Not Tissue: Mastering Laparoscopic Scissor Techniques & Types
In the fast-paced, high-stakes environment of modern minimally invasive surgery (MIS), every instrument in a surgeon’s hand is an extension of their skill and precision. Among these, Laparoscopic Scissors are indispensable tools for achieving the delicate balance between efficiency and safety, unlike traditional open surgery, where direct vision and tactile feedback guide the blade, laparoscopic cutting and dissection occur through small ports, viewed on a monitor, demanding an entirely different level of finesse. The ability to cut time, not tissue, is not merely a catchy phrase; it encapsulates the essence of effective laparoscopic surgery – swift yet accurate dissection that minimizes collateral damage and optimizes patient recovery.
This comprehensive guide will delve into the world of Laparoscopic Scissors, unraveling the complexities of their various types of laparoscopic scissors and, crucially, providing actionable strategies for mastering Laparoscopic Scissor techniques. We aim to empower surgeons to enhance their precision, reduce operative time, and, most importantly, uphold the highest standards of patient safety. By understanding the nuances of these instruments and applying proven techniques, surgical professionals can truly cut time, not tissue, and achieve superior outcomes in precision laparoscopic surgery.
The Edge of Innovation: What Are Laparoscopic Scissors?
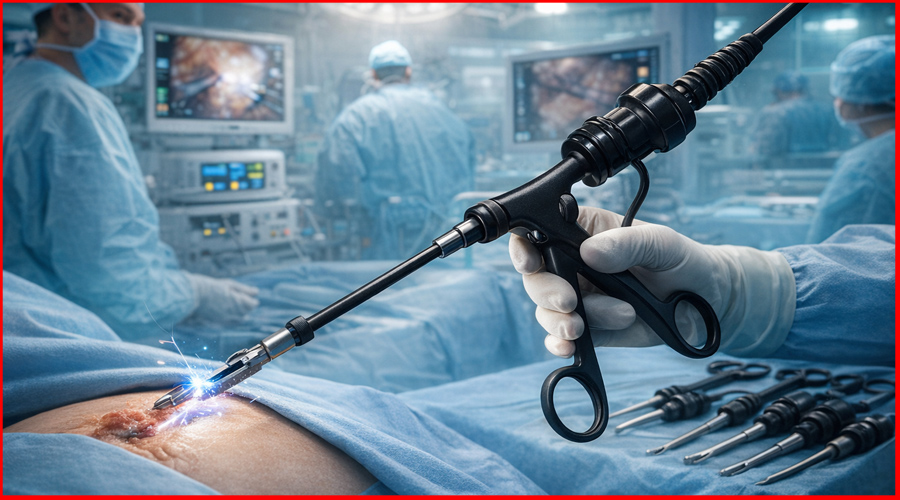
Laparoscopic Scissors are specialized surgical instruments designed for cutting and dissecting tissue within the confined space of the abdominal or thoracic cavity during minimally invasive procedures. They are the essential tools for sharp dissection, division of vessels (often after ligation), transecting organs, and preparing tissue planes.
A typical laparoscopic scissor comprises:
- The Jaws/Blades: These are the working ends, available in various configurations (straight, curved, hook) and often incorporate features for energy delivery (monopolar or bipolar). The sharpness and design of these blades are paramount for clean cuts and preventing tissue tearing.
- The Shaft is a long, slender tube (commonly 5mm or 10mm in diameter, with lengths ranging from 30cm to 45cm) that connects the blades to the handle. It typically includes insulation, particularly for energy-enabled scissors, and a rotation mechanism.
- The Handle/Finger Rings: The ergonomic grip for the surgeon, featuring a mechanism to open and close the blades. Handles can vary to optimize comfort and control.
The challenge with Laparoscopic Scissors is performing precise cuts without the direct tactile feedback of open surgery. Surgeons must rely heavily on visual cues from the monitor to gauge tissue tension, density, and proximity to vital structures. This reliance on visual feedback, coupled with the fulcrum effect of the port, necessitates mastering specific Laparoscopic Scissor techniques to ensure precision laparoscopic surgery.
Essential Types of Laparoscopic Scissors: Choosing Your Blade Wisely
The diverse array of types of Laparoscopic Scissors is not arbitrary; each design serves a specific purpose, contributing to the nuanced art of precision laparoscopic surgery. Understanding these variations is the first step in mastering Laparoscopic Scissor techniques and effectively achieving the goal to cut time, not tissue.
By Blade Configuration
The shape of the scissors blades dictates their primary function:
Straight Laparoscopic Scissors:
- Description: Features straight blades, similar to traditional open surgical scissors.
- Use: Excellent for direct, linear cutting of tissue, sutures, or mesh. They provide a straightforward visual reference for the cutting line.
- Precision Application: Ideal for clear, unobstructed areas where a direct cut is needed, or for suture cutting.
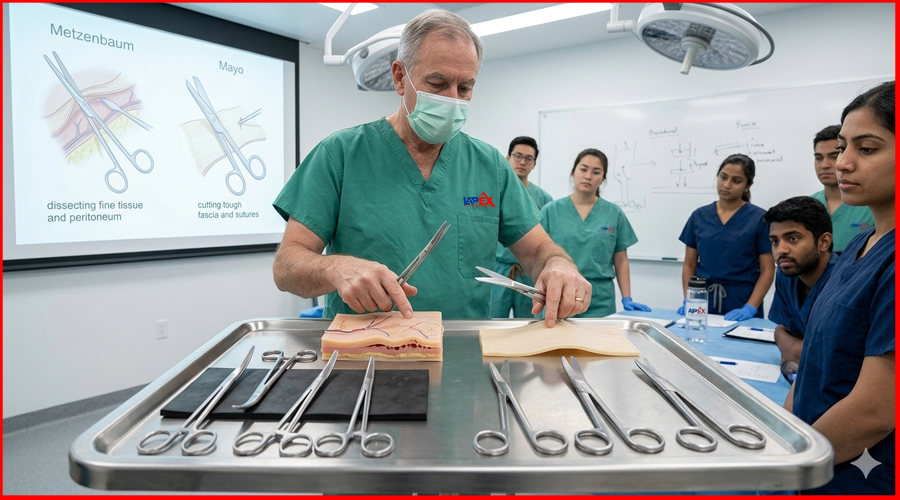
Curved Laparoscopic Scissors (Metzenbaum/Mayo-type):
- Description: The blades have a gentle or pronounced curve. Often thinner and more delicate (Metzenbaum-type) for fine dissection, or robust (Mayo-type) for tougher tissues.
- Use: The most versatile type for dissection. The curve allows for better visualization of the cutting plane by “pushing” tissue away, and facilitates blunt dissection when closed. They are excellent for dissecting around curved structures or creating planes.
- Precision Application: Highly favored for meticulous dissection around vessels, ducts, or nerves, allowing surgeons to follow anatomical contours and meticulously separate tissue planes. Essential for precision laparoscopic surgery.
Hook Scissors (e.g., J-Hook):
- Description: Features a distinctive hook-shaped tip, often with one blade ending in a hook and the other straight or slightly curved. Usually energy-enabled.
- Use: Primarily used for electrosurgical dissection. The hook allows for precise elevation and isolation of tissue before applying energy, minimizing unintended thermal spread. It excels at separating adhesions or dissecting around structures.
- Precision Application: Critical for controlled electrosurgical dissection, enabling surgeons to safely lift and cut tissue while applying energy, thereby reducing the risk of accidental thermal injury to adjacent vital structures. A key tool for cutting time, not tissue, by combining cutting and coagulation.
By Energy Modality
Many Laparoscopic Scissors integrate energy delivery for simultaneous cutting and coagulation (hemostasis), enhancing efficiency and safety.
- Monopolar Laparoscopic Scissors:
- Description: The active electrode is at the scissor tip. Current flows from the tip, through the patient, to a grounding pad.
- Use: Versatile for cutting and coagulating simultaneously. Excellent for rapid dissection of vascularized tissue.
- Safety Note: Requires careful insulation inspection as stray current can cause unintended burns away from the tip.
- Bipolar Laparoscopic Scissors:
- Description: Both active and return electrodes are within the scissor jaws. Current flows between the two blades, localizing the thermal effect.
- Use: Provides more localized coagulation, especially useful for smaller vessels where precise hemostasis is needed. Often preferred near critical structures due to reduced thermal spread.
- Safety Note: Generally considered safer than monopolar in terms of thermal spread, but blades need to be clean for effective coagulation.
By Material and Reusability
- Disposable Laparoscopic Scissors:
- Description: Single-use instruments, often made with sharper blades and guaranteed sterility.
- Advantages: Optimal sharpness every time, no concerns about cleaning or sterilization, and convenience.
- Disadvantages: Higher per-use cost, increased medical waste.
- Reusable Laparoscopic Scissors:
- Description: Designed for multiple uses after meticulous cleaning and sterilization.
- Advantages: More cost-effective long-term, reduced environmental impact.
- Disadvantages: Requires diligent cleaning and re-sterilization, potential for dulling over time (requiring resharpening), increased risk of damage with repeated use.
A deep understanding of these types of Laparoscopic Scissors allows a surgeon to select the perfect instrument for each specific dissecting or cutting task, which is fundamental to mastering Laparoscopic Scissor techniques and achieving precision laparoscopic surgery.
Mastering Laparoscopic Scissor Techniques: Cut Time, Not Tissue
Achieving proficiency with Laparoscopic Scissors transcends simply knowing the types; it involves developing refined techniques that allow for efficient, precise, and safe tissue manipulation. This is where the true art of “cut time, not tissue” lies.
The Two-Handed Approach: Dissection Synergy:
- Core Principle: Laparoscopic dissection is almost always a two-instrument maneuver. One hand (often the non-dominant hand) manipulates a grasper to provide counter-traction, while the other hand uses the Laparoscopic Scissors for cutting or blunt dissection.
- Benefit: Counter-traction stretches the tissue, making planes more visible and creating tension that allows for cleaner, more precise cuts. This minimizes tearing and uncontrolled movements, significantly contributing to precision laparoscopic surgery.
Visual Acuity: “If You Can’t See It, Don’t Cut It”:
- Challenge: The loss of direct tactile feedback in laparoscopy means visual input is paramount.
- Technique: Always ensure the entire length of the scissor blades and the tissue to be cut are visible on the monitor. If smoke, blood, or surrounding tissue obstructs the view, clear it with suction/irrigation or reposition the camera. Never make a blind cut. This is the foundational rule for Laparoscopic Scissor safety.
Controlled Force Application:
- Balance: Apply just enough force to cut through the tissue cleanly. Too little force leads to tearing or crushing, while too much force can cause the blades to “pop through” unpredictably, risking injury to underlying structures.
- Practice: Develop an intuitive feel for tissue resistance through the instrument’s handle by practicing on simulators with varying tissue densities.
The Fulcrum Effect and Angle of Attack:
- Understanding: The trocar site acts as a fulcrum. A small movement of the handle outside results in a larger, opposite movement of the blades inside.
- Technique: Anticipate this magnified movement. For precise cuts, often a gentle, minimal movement of the handle is required. Adjust your angle of attack so that the blades are parallel to the desired cutting line, and the tips are visible throughout the cut.
Blunt vs. Sharp Dissection (with Curved Scissors):
- Blunt Dissection: Use the closed or partially opened blades of curved laparoscopic scissors to gently push and separate tissue along natural planes, preserving vessels and nerves. This technique allows for meticulous identification of structures.
- Sharp Dissection: Once planes are identified, open the blades to make precise cuts. The curve helps to elevate tissue, allowing the surgeon to see what is behind the cutting edge.
“Painting” with Hook Scissors (Energy Dissection):
- Technique: When using a J-hook or similar energy-enabled scissor, use short, controlled bursts of energy. Instead of long, sweeping cuts, “paint” the tissue with the hook, elevating small sections and applying energy only when the tissue is isolated and visible. This minimizes thermal spread and enhances Laparoscopic Scissor safety.
Suture Cutting Technique:
- When cutting sutures, orient the scissor blades perpendicularly to the suture thread. Position the blades close to the knot, ensuring you cut only the suture and not the underlying tissue. Close the blades fully and pull the suture through the fully closed blades for a clean cut.
Efficient Blade Cleaning:
- During prolonged procedures, especially with energy-enabled scissors, eschar (burnt tissue) can accumulate on the blades, reducing cutting efficiency and increasing thermal spread. Periodically clean the blades by wiping them against a gauze sponge or a specialized cleaning pad delivered through a port. This maintains sharpness and improves Laparoscopic Scissor safety.
Continuous Practice:
- Mastery is a journey. Regular practice on laparoscopic simulators (box trainers, VR) or in cadaver labs is essential. Focus on repetitive movements, precision tasks (e.g., cutting a precise circle), and integrating both hands fluidly. This deliberate practice is the ultimate key to mastering Laparoscopic Scissor techniques and truly being able to “cut time, not tissue.”
Avoiding Surgical Errors: Key Laparoscopic Scissor Safety Tips
While Laparoscopic Scissors are tools for efficiency, their improper use can lead to significant surgical errors. Adhering to strict safety protocols is paramount for precision laparoscopic surgery and protecting the patient.
Always visualize the Blades: This is the most critical safety rule. If the tips of your Laparoscopic Scissors are not in clear view on the monitor, stop immediately. Reposition the camera, adjust your angle, or even withdraw and reinsert the instrument until full visualization is achieved. Blind cuts are a leading cause of iatrogenic injury.
Identify Tissue Before Cutting: Before making any cut, unequivocally identify the tissue you are about to divide. Use grasping forceps to confirm its identity, separate it from adjacent structures, and ensure no vital structures (e.g., bowel, ureter, major blood vessels, nerves) are in the path of the blades. This is a non-negotiable step for Laparoscopic Scissor safety.
Inspect Insulation (Energy Scissors): For monopolar or bipolar Laparoscopic Scissors, meticulously inspect the insulation along the entire shaft before insertion and periodically during the procedure. Even a tiny breach in the insulation can lead to “stray current” burns to adjacent tissue, which can be devastating and often go unnoticed until complications arise post-operatively.
Controlled Cutting Motion: Apply steady, controlled pressure when closing the blades. Avoid sudden, jerky movements, which can cause the blades to “jump” or “pop through” tissue unexpectedly, leading to unintended cuts or perforations.
Avoid Using Scissors as Graspers: While tempting to quickly grab something with the scissors jaws, repeatedly using them as graspers can dull the blades, compromise their alignment, and reduce their cutting efficiency. Always use appropriate grasping forceps for tissue manipulation.
Beware of Thermal Spread (Energy Scissors): Understand the zone of potential thermal spread when using energy-enabled scissors. Ensure there is adequate distance between the energized blade and vital structures. Use short, controlled bursts of energy rather than prolonged activation.
Manage Smoke and Bleeding: Smoke from energy devices and blood can obscure the view. Use effective suction and irrigation to maintain a clear operative field. A clear view is fundamental for precision laparoscopic surgery.
Controlled Entry and Exit: Insert and withdraw the Laparoscopic Scissors smoothly through the trocar. Avoid rapid or forceful movements, which can snag or tear tissue at the port site or within the abdominal cavity.
Prevent Instrument Clashing: Be aware of the spatial relationship between your instruments and the camera. Avoid clashing instruments inside the body, which can damage the blades or insulation or obscure the view.
Regular Maintenance and Sharpening: For reusable scissors, ensure they undergo meticulous cleaning, sterilization, and regular professional maintenance/resharpening. Dull scissors tear rather than cut, increasing tissue trauma and risk of injury. This is a crucial aspect of Laparoscopic Scissor safety.
Conceptual Comparison Table: Types of Laparoscopic Scissors
To aid in selecting the most appropriate instrument for different surgical scenarios, here’s a conceptual comparison table outlining the key features and applications of common types of Laparoscopic Scissors:
| Scissor Type | Blade Features | Energy Option | Primary Use | Key Advantage for Precision | Considerations |
|---|---|---|---|---|---|
| Straight | Straight blades, pointed tip | Often Monopolar | Linear cutting, suture cutting | Direct, intuitive cutting in open planes | Limited for curved dissection, can be dull faster |
| Curved | Curved blades, blunt or sharp tips | Often Monopolar/Bipolar | Dissection along curves, blunt dissection, creating planes | Facilitates dissection around structures and better visualization of the cutting plane | Requires more skill for precise straight cuts |
| Hook (J-Hook) | Hooked tip, one blade often blunt | Monopolar (most common) | Precise energy dissection, adhesion lysis | Elevates and isolates tissue for precise energy application; minimizes thermal spread | Primarily for energy use; not for blunt dissection or mechanical cutting |
| Metzenbaum | Delicate, thin blades, usually curved | Often non-energy, sometimes bipolar | Fine dissection, delicate tissue separation | Minimal tissue trauma, excellent for precise plane development | Less robust for thick tissue or major vessels |
| Mayo | Robust, strong blades, often curved | Often non-energy | Cutting thick tissue, sutures, and mesh | Strength for tough structures | Can be too traumatic for delicate dissection |
Laparoscopic Scissors are far more than simple cutting tools in the minimally invasive surgery toolkit. They are sophisticated instruments that, when wielded with mastery, enable surgeons to achieve unparalleled levels of precision and efficiency. The ability to “cut time, not tissue” is the hallmark of a skilled laparoscopic surgeon, signifying swift yet meticulous dissection that respects tissue integrity and promotes optimal patient recovery.
By thoroughly understanding the various types of Laparoscopic Scissors – from their blade configurations to their energy capabilities – and by diligently applying refined Laparoscopic Scissor techniques, surgeons can significantly enhance their performance. This includes mastering the two-handed approach, ensuring absolute visual control, and making deliberate, controlled movements. Crucially, a relentless commitment to Laparoscopic Scissor safety through vigilant inspection and adherence to established protocols is non-negotiable. Ultimately, true mastery of Laparoscopic Scissors is a continuous journey of learning and practice, leading to safer, more efficient, and more precise surgical outcomes for every patient.
For more information, feel free to contact the Lapex Surgical support team.