Table of Contents
ToggleUnderstanding Electrosurgical Waveforms: A Surgeon’s Guide to Cut, Coagulate, & Blend
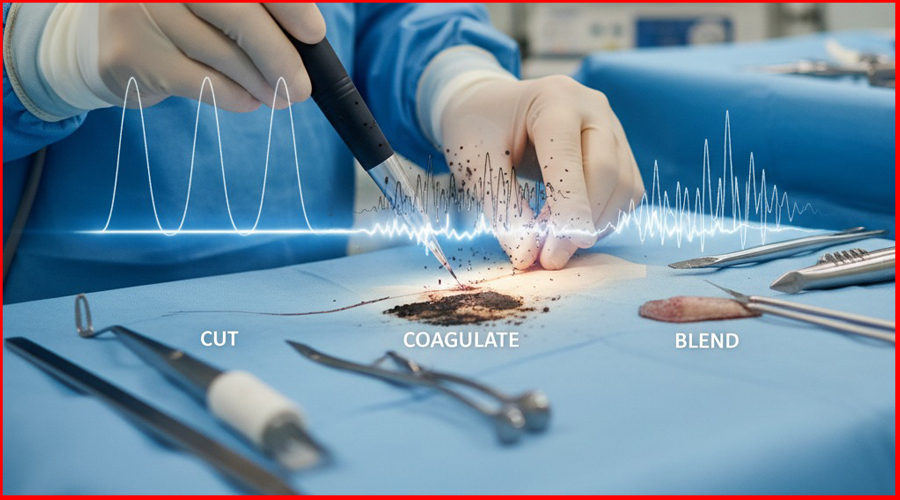
In the modern operating room, few tools offer the versatility and precision of an electrosurgical instrument. With a single device, a surgeon can meticulously dissect tissue, staunch bleeding, and perform a combination of both. This remarkable ability, however, is not magic. It is the result of a precise manipulation of electrical current, governed by an unseen force—the electrosurgical waveform.
For surgeons, understanding the science behind these waveforms is a critical skill. It’s the difference between a clean, controlled incision and unintended tissue damage. It’s the key to achieving optimal hemostasis and minimizing thermal spread. For manufacturers like Lapex Surgical, it is the very foundation of our product design.
This article will demystify the technical aspects of electrosurgery, providing a comprehensive guide to the different waveforms that empower the surgeon’s hand. We’ll delve into the basic principles, break down the distinct characteristics of cutting and coagulation modes, explore the versatility of blend settings, and explain how the right instrument, like those from Lapex Surgical, is engineered to perfectly deliver these effects.
1. The Invisible Force: Basic Principles of Electrosurgery
At its core, electrosurgery is the application of high-frequency electrical current to biological tissue to generate a desired thermal effect. The key term here is high frequency. Unlike the low-frequency current that powers your household appliances and can cause neuromuscular stimulation (e.g., a shock), electrosurgical units (ESUs) operate at frequencies typically above 100 kHz. At these frequencies, the current no longer excites nerves and muscles, instead converting the electrical energy into heat as it passes through the tissue’s resistance.
This thermal effect is a direct result of cellular resistance. As the current travels from the active electrode (the instrument tip) and passes through the cells, it generates heat. The speed and intensity of this heat generation are what determine the tissue’s reaction—either vaporization, desiccation, or fulguration.
The process involves a simple, yet elegant, circuit:
The ESU Generator: The “brain” of the system, which produces the high-frequency current and allows the surgeon to select the power level and waveform.
The Active Electrode: The working instrument, such as an electrosurgical pencil, forceps, or scissors, that delivers the current to the surgical site.
The Patient: The tissue itself, which acts as the resistor in the circuit.
The Return Electrode: A grounding pad placed on the patient’s body that safely collects the current and returns it to the ESU, completing the circuit.
The true magic, however, lies in how the ESU shapes the electrical signal. This is where waveforms come into play, each with a unique purpose.
2. The Cutting Waveform: Precision and Vaporization
When a surgeon needs to make a clean, precise incision, they select the cutting mode. This mode relies on a waveform that is carefully designed to vaporize tissue almost instantaneously.
The Anatomy of a Cutting Waveform
A cutting waveform is a high-voltage, continuous, unmodulated sinusoidal wave.
Continuous: The waveform is uninterrupted, meaning the electrical current flows constantly. This allows for a steady delivery of energy.
High Voltage: The peaks of the voltage are high, which causes the cellular water inside the tissue to rapidly heat and turn to steam. This rapid expansion of steam causes a localized cellular explosion.
Unmodulated: The signal is a pure sine wave, which delivers a consistent flow of energy.
The Thermal Effect: Cellular Vaporization
The high-voltage, continuous current causes the temperature of the cells directly in the current’s path to rise so quickly that the water inside them boils and expands explosively. This rapid cellular rupture creates a very fine, narrow incision with minimal collateral thermal damage to the surrounding tissue. It’s akin to a hot knife slicing through butter—the heat is so concentrated at the point of contact that it causes a smooth separation with little spreading of the effect.
Clinical Application: The cutting waveform is ideal for:
Incision and Dissection: Making clean, precise cuts through skin, muscle, or other tissues.
Tissue Excision: Removing a specific mass or specimen with a well-defined margin.
Minimizing Tissue Drag: The rapid vaporization effect creates a smooth cut with minimal resistance.
The cutting mode is the go-to for surgical dissection when a clean, bloodless cut is required and hemostasis is not the primary goal.
3. The Coagulation Waveform: The Power of Desiccation
In contrast to cutting, coagulation is all about stopping bleeding. The waveform for this mode is engineered to achieve a different thermal effect: desiccation, or the drying out of tissue.
The Anatomy of a Coagulation Waveform
A coagulation waveform is a low-voltage, intermittent, high-frequency signal.
Intermittent: The waveform is not continuous. It is delivered in short, high-energy bursts with significant pauses in between. This allows heat to build up slowly within the tissue without causing vaporization.
Low Voltage: The voltage is lower than the cutting waveform. This prevents the rapid, explosive effect of vaporization.
High-Frequency: The bursts are delivered at a high frequency, ensuring that the current still generates heat in the tissue.
The Thermal Effect: Cellular Desiccation
The intermittent bursts of current cause the tissue to heat up gradually. This slower, less explosive heating drives the water out of the cells, causing them to shrink and shrivel. This process, known as desiccation, seals small blood vessels by coagulating the proteins within the vessel walls. The result is hemostasis, or the cessation of bleeding. The tissue effect is a white, dry appearance, and there is more lateral thermal spread than with the cutting waveform.
Clinical Application: The coagulation waveform is essential for:
Hemostasis: Sealing small blood vessels to control bleeding.
Spot Coagulation: Stopping bleeding from specific points on tissue surfaces.
Reducing Blood Loss: A fundamental tool for achieving a clear surgical field.
The coagulation mode is the surgeon’s tool for controlling bleeding, which is a constant challenge in every procedure.
4. The Art of the Blend: Combining Cut and Coag
The true versatility of electrosurgery lies in the ability to blend the cutting and coagulation effects. A blend mode is created by an ESU that modulates the waveform, mixing the continuous cutting waveform with the pulsed coagulation waveform.
How Blend Modes Work
An ESU’s blend setting is a simple function of its duty cycle—the percentage of time the waveform is in its “on” state. The standard cutting mode has a 100% duty cycle, while the coagulation mode might have a duty cycle as low as 6% to 10%. A blend mode is a combination of these two extremes.
Blend 1: A high percentage of cutting time (e.g., 80%) and a small percentage of coagulation time (e.g., 20%). The tissue effect is primarily a clean cut with a slight amount of hemostasis.
Blend 2: A more balanced blend (e.g., 50% cutting, 50% coagulation). This provides a moderate cut with a good level of hemostasis.
Blend 3: A higher percentage of coagulation time (e.g., 25% cutting, 75% coagulation). This provides a slower cut with excellent hemostasis.
Blend Mode | Waveform Characteristic | Primary Tissue Effect | Clinical Application |
|---|---|---|---|
Pure Cut | Continuous, High Voltage | Vaporization | Precise incision, tissue dissection |
Blend 1 | Modulated, 80% Cut | Cut with minimal coagulation | Dissection in highly vascular tissue |
Blend 2 | Modulated, 50% Cut | Cut with moderate coagulation | All-purpose cutting and hemostasis |
Blend 3 | Modulated, 25% Cut | Slower cut with high coagulation | Slower dissection with significant bleeding control |
Pure Coagulation | Intermittent, Low Voltage | Desiccation | Hemostasis, sealing vessels |
Clinical Applications of Blend Modes
Blend modes are invaluable for surgeons operating in highly vascular areas where bleeding can obscure the surgical field. For instance, in an abdominal surgery where the surgeon must cut through a lot of fatty tissue with many small vessels, a blend mode allows them to progress with their dissection while simultaneously sealing off bleeders, maintaining a clear view. It streamlines the procedure by reducing the need to switch between two separate instruments or modes.
5. The Role of the ESU and Proper Settings
The electrosurgical unit is the heart of the system, but the surgeon is its conductor. Properly setting the ESU is a critical skill that impacts every aspect of the procedure.
Power Setting: The power (measured in watts) determines the intensity of the effect. A lower wattage is used for delicate work, while a higher wattage may be needed for cutting through denser tissue. The key is to use the lowest effective power setting to minimize collateral thermal damage.
Mode Selection: The surgeon selects the desired waveform (Cut, Coag, or Blend) based on the specific tissue and the goal of the moment. Many modern electrosurgical pencils have integrated finger-switches that allow the surgeon to toggle between modes without looking away from the surgical field, a key feature for efficiency and safety.
Patient Return Electrode Monitoring: For monopolar systems, ensuring the return pad is properly placed and its contact is monitored is crucial. A poor connection can concentrate the current at the point of contact, leading to a serious patient burn.
A high-quality ESU will offer precise, reliable control over these settings. However, the true performance of the system relies on the quality of the instruments attached to it.
6. The Lapex Surgical Advantage: Optimized for Performance
At Lapex Surgical, we don’t just manufacture surgical tools; we engineer a complete solution. Our electrosurgical instruments are meticulously designed to work in perfect harmony with the ESU and its various waveforms, ensuring that the surgeon’s intent is perfectly translated into the desired tissue effect.
Precision Tip Design
The shape and material of the active electrode tip are paramount. Whether it’s a fine needle tip for precise cutting, a robust blade for broad incisions, or a ball tip for effective coagulation, our instruments are crafted to deliver the current with pinpoint accuracy. The quality of our German stainless steel and the precision of our milling processes ensure that the tip’s surface and geometry remain consistent, guaranteeing reliable performance.
Ergonomics and Control
A surgeon’s hand should be an extension of their will. Our electrosurgical pencils are designed with ergonomic comfort in mind, reducing hand fatigue during long procedures. The integrated finger-switches are intuitively placed and responsive, allowing for instant and seamless switching between cut and coagulation modes. This fluid control ensures that the surgeon can react to the needs of the tissue in real-time without interruption.
The Non-Negotiable of Insulation Integrity
As we discussed in a previous article, the insulation on our electrosurgical instruments is non-negotiable. For a waveform to deliver its intended effect safely, the current must be perfectly contained until it reaches the active tip. Our durable, high-dielectric insulation, coupled with our stringent electrical integrity testing, guarantees that the surgeon can trust the instrument implicitly, preventing unintended current leakage and devastating patient burns.
The right instrument is the final link between the ESU’s waveform and the patient’s tissue. A poorly designed or manufactured instrument can compromise even the most advanced ESU, leading to unpredictable results. Lapex Surgical’s unwavering commitment to quality ensures that our instruments are always up to the task, providing a reliable channel for the precise delivery of power.
Conclusion
The power of electrosurgery lies not in brute force, but in the elegant science of waveforms. By understanding the distinct characteristics of cutting, coagulation, and the various blend modes, surgeons can harness this technology with greater precision and confidence. The high-voltage, continuous waveform of the cutting mode enables meticulous dissection, while the low-voltage, intermittent waveform of coagulation provides unmatched hemostasis. The art of blending these modes offers unparalleled versatility in complex surgical scenarios.
At Lapex Surgical, we are proud to be at the intersection of this technology and timeless craftsmanship. Our instruments are more than just metal and plastic; they are meticulously engineered tools designed to perfectly deliver the science of these waveforms. We believe that by providing surgeons with tools that embody this level of understanding, we empower them to achieve the highest standards of surgical excellence, ensuring better outcomes for patients worldwide.
Frequently Asked Questions (FAQ)
Q1: What is the main difference between monopolar and bipolar electrosurgery?
A1: In monopolar electrosurgery, the current flows from the active electrode, through the patient, to a return pad. In bipolar electrosurgery, the current flows only between the two tips of the instrument (e.g., bipolar forceps), making it safer for use near sensitive structures and in patients with pacemakers.
Q2: Why is the ESU's frequency important?
A2: The frequency is critical because it determines whether the current causes neuromuscular stimulation (a shock). At the high frequencies (above 100 kHz) used in electrosurgery, the current passes through the body without shocking the patient, allowing it to be used for thermal effects.
Q3: What does it mean for a waveform to be "modulated"?
A3: A modulated waveform is one whose amplitude or frequency is varied over time. In electrosurgery, modulation is used to create blend modes by interrupting the continuous cutting waveform with pauses, thereby creating a combined effect of cutting and coagulation.
Q4: Can I use the same power setting for both cutting and coagulation?
A4: While some general guidelines exist, it is not recommended to use the same power setting for both modes. Each waveform is designed for a specific purpose, and the optimal power setting will depend on the tissue type, the desired effect, and the specific ESU and instrument being used. Always follow the manufacturer’s guidelines.
Q5: How does Lapex Surgical ensure its electrosurgical instruments are optimized for waveform delivery?
A5: Lapex Surgical’s instruments are designed with a focus on premium materials, precision-engineered tips, ergonomic handles, and robust insulation. This attention to detail ensures optimal conductivity, consistent tissue interaction, and secure current containment, allowing the surgeon to confidently deliver the precise waveform effect.
Q6: What is "fulguration" and how does it relate to coagulation?
A6: Fulguration is a type of non-contact coagulation. It occurs when a spark jumps from the electrode tip to the tissue, causing a superficial carbonization and sealing of small vessels. This is a very effective way to achieve hemostasis over a broader area without direct contact with the tissue.