Table of Contents
ToggleLaparoscopic Graspers: Master Precision & Avoid Surgical Errors with These Proven Tips
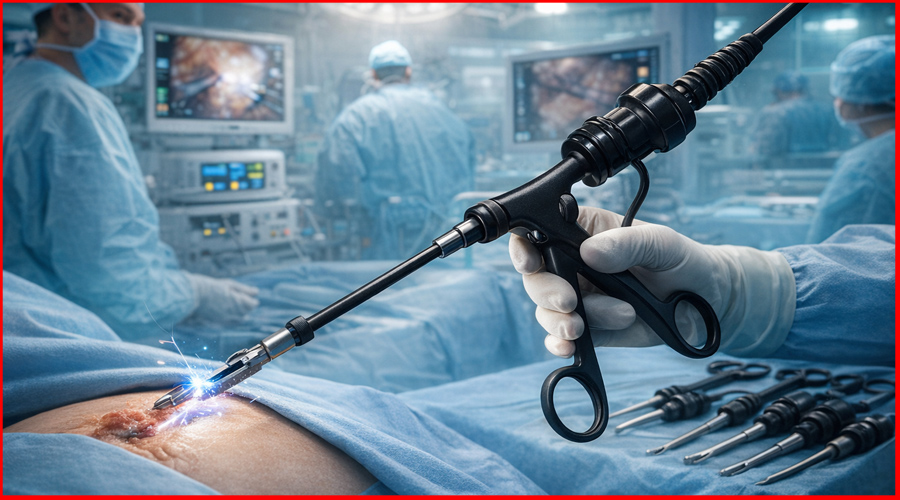
In the intricate world of laparoscopic surgery, where surgeons operate through small incisions while viewing their work on a monitor, precision is not just a goal – it’s an absolute necessity. Among the diverse array of specialized tools, Laparoscopic Graspers are the surgeon’s primary extension into the patient’s body, serving as their “hands” to hold, manipulate, and retract delicate tissues. The quality of these instruments, coupled with the surgeon’s mastery in their use, directly dictates the safety and success of the procedure.
Unlike open surgery, where tactile feedback is direct and immediate, laparoscopic surgery introduces challenges like 2D vision (without depth perception unless using 3D systems) and the loss of direct touch sensation. This means that every movement, every grasp, and every release with Laparoscopic Graspers must be executed with unparalleled accuracy. A misplaced grip or an uncontrolled force can lead to significant complications and surgical errors.
This comprehensive guide is designed for surgeons, residents, and anyone interested in the nuances of minimally invasive surgery. We will delve into the types of Laparoscopic Graspers, explore essential tips to master precision laparoscopic graspers, and provide actionable strategies to avoid surgical errors stemming from instrument handling effectively. By understanding and applying these proven techniques, surgical professionals can elevate their performance, optimize patient outcomes, and enhance the overall safety of laparoscopic procedures.
The Unsung Heroes: Understanding Laparoscopic Graspers
Laparoscopic Graspers are arguably the most versatile and frequently used instruments in minimally invasive surgery. They are the workhorses of the laparoscopic operating room, performing myriad functions that mimic the human hand, but through a long, slender shaft.
A typical laparoscopic grasper consists of three main components:
- The Jaws/Tips: These are the working ends of the instrument, designed with various shapes, sizes, and serrations (or lack thereof) to interact with different types of tissue.
- The Shaft: This is the long, thin rod that connects the jaws to the handle, allowing the instrument to reach deep into the body through a small port. Most shafts also allow for 360-degree rotation.
- The Handle/Finger Rings: This is the part held by the surgeon, equipped with a mechanism (often a scissor-like handle or a pistol grip) that controls the opening and closing of the jaws. A locking mechanism is often present to maintain a grip without continuous pressure.
The effectiveness of laparoscopic surgery hinges on the ability of these graspers to perform their tasks precisely, securely, and atraumatically. From gently retracting an organ to firmly holding a suture, the correct selection and masterful handling of these instruments are directly linked to the success of the surgical intervention and the prevention of surgical errors. Their design variations are critical, as using the wrong grasper can quickly turn a delicate maneuver into a damaging event.
Types of Laparoscopic Graspers: Choosing the Right Tool
One of the foundational principles in avoiding surgical errors in laparoscopic surgery is the judicious selection of the appropriate instrument for the task at hand. The vast array of Laparoscopic Graspers is not merely for variety; each design is tailored for specific tissue types and surgical maneuvers. Understanding these distinctions is crucial for mastering precision laparoscopic graspers.
By Jaw Design (Focus on Tissue Interaction)
The design of the grasper’s jaws dictates how it interacts with tissue, making this the most critical differentiation.
Atraumatic Graspers:
- Description: These graspers are characterized by smooth, blunt, or finely serrated jaws that are designed to minimize tissue damage. They often have a “fenestrated” (windowed) design, which means there are openings in the jaws to allow fluids to pass through and to reduce the surface area contact, thus distributing pressure more evenly.
- Use: Ideal for handling delicate structures such as bowel, bladder, major blood vessels, or thin mesentery where crushing or tearing must be avoided. They are commonly used for gentle retraction to expose the surgical field. Using an atraumatic grasper when handling sensitive tissue is a primary method to avoid surgical errors related to inadvertent damage.
- Examples: Babcock graspers (broad, fenestrated, gentle), DeBakey graspers (long, fine, non-fenestrated serrations).
Traumatic / Toothed Graspers:
- Description: These graspers feature sharp teeth or prominent serrations on their jaws.
- Use: Designed for securely grasping dense tissue, fascia, or large specimens that are being removed from the body. Their teeth provide a very firm grip, which can be essential when significant traction is needed. However, they must be used with extreme caution and never on delicate or vital structures due to the high risk of tissue damage, perforation, or bleeding. Improper use is a common cause of surgical errors.
- Examples: Alligator forceps (fine, sharp teeth), some large tissue-grasping forceps.
Fenestrated vs. Non-Fenestrated Graspers:
- Fenestrated: Have “windows” or openings in the jaws. They allow visibility of the tissue within the jaws and prevent “tenting” of tissue and fluid accumulation, offering a gentler, more compliant grip.
- Non-Fenestrated: Jaws are solid. They provide a more continuous, broader surface contact and can be useful for dissection or pushing tissue.
By Function (Specific Applications)
Beyond basic grasping, many Laparoscopic Graspers are specialized for particular surgical actions.
- Dissecting Graspers (e.g., Maryland Dissector):
- Description: Often feature a curved, blunt tip with fine serrations. Many are monopolar compatible, meaning they can be connected to an electrosurgical unit for cautery (cutting and sealing tissue with heat).
- Use: The workhorse for blunt dissection (separating tissues along natural planes) and some sharp dissection. The curved tip allows for efficient “hooking” and separation of tissue. Their versatility makes them crucial for mastering precision laparoscopic graspers.
- Babcock Graspers:
- Description: A classic type of atraumatic grasper with distinctive, broad, fenestrated jaws that form a circular shape when closed.
- Use: Specifically designed for holding delicate, tubular structures like bowel, fallopian tubes, or appendix without causing significant crushing injury.
- Kelly Forceps / Crile Forceps (Laparoscopic Versions):
- Description: Resemble their open surgery counterparts, with straight or curved jaws featuring horizontal serrations.
- Use: General grasping, clamping small vessels, or passing sutures.
- Right-Angle Dissectors:
- Description: Features a right-angle bend at the tip, often with a fine, blunt, or serrated jaw.
- Use: Ideal for reaching around structures to dissect or to clamp vessels in tight spaces that are difficult to access directly.
Choosing the precise grasper for each step of the surgery is the first, and perhaps most critical, proven tip in the journey to master precision laparoscopic graspers and avoid surgical errors. It significantly reduces the risk of iatrogenic (surgeon-caused) injury.
Proven Tips to Master Precision Laparoscopic Graspers
Achieving mastery with Laparoscopic Graspers requires more than just knowing their types; it demands deliberate practice and adherence to fundamental principles. These tips are designed to enhance your skills and contribute significantly to avoiding surgical errors.
Instrument Selection is Paramount:
- Always begin by confirming you have the correct grasper type for the intended tissue and task. Attempting to dissect delicate structures with a traumatic grasper is an invitation for injury. Conversely, using an overly gentle grasper for dense tissue will lead to frustration and inefficiency.
- For example, when retracting the bowel, always opt for an atraumatic Babcock or fenestrated grasper. When dissecting around critical vessels, the Maryland dissector is often preferred. This conscious choice is the first line of defense against surgical errors.
Ergonomics and Grip Optimization:
- How you hold the grasper directly impacts your control and precision. Avoid a “death grip” that can lead to fatigue and jerky movements.
- Finger Placement: Ensure your fingers are comfortably positioned in the rings, allowing for a full range of motion. The thumb and index finger typically control the primary jaw movement, while the middle or ring finger provides stability.
- Wrist Position: Maintain a neutral wrist position as much as possible to reduce strain and allow for fluid, controlled movements. Awkward wrist angles compromise fine motor control.
The “Two-Handed” Approach:
- Laparoscopic surgery is inherently a two-handed operation. The most effective way to master precision laparoscopic graspers is to utilize both instruments in a coordinated dance.
- One grasper often provides counter-traction, while the other performs dissection or manipulation. This synergistic action creates tension planes that allow for cleaner dissection and safer handling of tissue. Never rely on one hand to do all the work if two hands can be used.
Leverage and the Fulcrum Effect:
- The laparoscopic port acts as a fulcrum. Understanding this means that a small movement of the grasper handle outside the body translates to a larger, opposite movement of the tip inside the body. This is crucial for mastering precision laparoscopic graspers.
- Practice compensating for this effect. For instance, to move the tip a small amount to the right, you might need to move the handle a larger amount to the left. This requires deliberate practice.
Mastering Depth Perception (2D Vision Strategies):
- In traditional 2D laparoscopic vision, depth perception is lost. Overcoming this is key to avoiding surgical errors.
- Triangulation: Position your instruments and camera to form a triangle with the target tissue. This provides visual cues that help estimate depth.
- “Fingering” Tissue: Gently touching tissue with the grasper tip can provide subtle visual feedback on its texture, density, and 3D position, mimicking tactile sensation.
- Shadows: Utilize the light source to create shadows that reveal depth.
- Relative Movement: Observe how instruments move relative to each other and fixed anatomical landmarks to gauge depth.
Controlled Force Application:
- Without direct tactile feedback, it’s easy to apply too much or too little force. Learning to feel the appropriate tension through the handle’s resistance is a refined skill.
- Practice on Simulators: Use box trainers or virtual reality simulators to practice grasping various simulated tissues until you develop an intuitive understanding of appropriate force. Excessive force can cause unseen tissue trauma and lead to surgical errors.
Counter-Traction: The Dissector’s Best Friend:
- When dissecting, always ensure adequate counter-traction. This means pulling the tissue in one direction with one grasper while dissecting or pushing in the opposite direction with the other. This creates a taut plane that allows for cleaner, safer dissection and reduces the risk of accidental injury to adjacent structures. It’s fundamental to master precision laparoscopic graspers.
Camera Synchronization: “Follow the Tip”:
- The surgeon operating the camera (or the robotic system) must constantly synchronize the camera’s view with the movements of the grasper tips. The grasper’s working end should always be in the center of the screen, allowing for clear visualization of the action. This coordinated movement is vital for preventing loss of view and potential surgical errors.
Regular Instrument Inspection (Pre-Case):
- Before every procedure, personally inspect all Laparoscopic Graspers. Check for:
- Jaw alignment: Ensure the jaws meet perfectly and close flush.
- Serration integrity: Confirm that teeth or serrations are not bent or broken.
- Shaft integrity: Look for bends, nicks, or insulation breaks (especially if used with energy).
- Handle functionality: Check for smooth opening/closing, locking mechanism, and rotation.
- A faulty instrument can lead to catastrophic surgical errors. This simple step is non-negotiable.
- Before every procedure, personally inspect all Laparoscopic Graspers. Check for:
Practice, Practice, Practice:
- Mastery is a journey, not a destination. Regular practice on:
- Box Trainers: Low-cost, effective for developing basic skills and hand-eye coordination.
- Virtual Reality (VR) Simulators: Offer immersive, realistic scenarios with performance metrics.
- Animal Labs or Cadaver Courses: Provide the most realistic tissue handling experience.
- Consistent, deliberate practice is the cornerstone for anyone aspiring to master precision laparoscopic graspers.
- Mastery is a journey, not a destination. Regular practice on:
Avoiding Surgical Errors with Laparoscopic Graspers: A Safety Checklist
Beyond mastering precision, specific safety protocols when handling Laparoscopic Graspers are paramount to avoid surgical errors and ensure optimal patient outcomes. This checklist serves as a reminder of crucial considerations during a procedure.
- Always Identify Your Tissue: Never grasp or apply energy to tissue without absolutely confirming its identity. Distinguishing bowel from omentum, or a critical vessel from a benign structure, is fundamental. If in doubt, dissect more to confirm.
- Electrocautery Insulation Integrity: If using a monopolar grasper, meticulously inspect the insulation along the shaft before and during the procedure. A break in insulation can lead to unintended burns (“stray current”) to adjacent structures, causing potentially devastating surgical errors that may not be immediately visible.
- Port Site Awareness: Always be aware of where your instrument is entering and exiting the abdominal wall. Avoid “fencing,” where instruments cross excessively outside the body, leading to awkward movements and potential tearing at the port site or instrument entanglement inside.
- Never Grasp Blindly: The tips of your Laparoscopic Graspers should always be visible on the monitor. If you lose sight of the tips, stop all movement, reorient the camera, or withdraw and reinsert the instrument until you regain full visualization. “If you can’t see it, don’t do it” is a golden rule.
- Controlled Instrument Removal: When withdrawing a grasper, do so smoothly and carefully. Rapid or uncontrolled withdrawal can snag or tear tissue at the port site or on the abdominal wall. Ensure jaws are closed or nearly closed when withdrawing.
- Optimal Patient Positioning: Work with the anesthesia team to ensure the patient is optimally positioned. Proper positioning can improve anatomical exposure, enhance instrument maneuverability, and reduce strain on the surgeon, thereby contributing to fewer surgical errors.
- Protocol for Instrument Malfunction: Have a clear plan for what to do if a grasper jams, breaks, or malfunctions mid-procedure. This includes having backup instruments readily available and knowing the protocol for safe removal of a broken instrument part if necessary.
- Clear Communication with the Surgical Team: Maintain open lines of communication with your scrub technician, circulating nurse, and surgical assistant. Clearly articulate which grasper you need, when you need it, and if any issues arise. This collaborative approach enhances efficiency and safety.
Instrument Care and Maintenance: Protecting Your Investment
The longevity and performance of Laparoscopic Graspers are directly tied to how well they are cared for. Proper instrument care and maintenance are not just about prolonging the life of expensive tools; they are vital for ensuring the instruments perform optimally during surgery, which directly impacts patient safety and helps avoid surgical errors. This also significantly affects the Cost-effectiveness of Laparoscopic Instruments.
- Immediate Post-Operative Cleaning: Instruments should be wiped down immediately after use to prevent blood and tissue from drying onto surfaces. This makes subsequent cleaning much easier and more effective.
- Thorough Cleaning and Disinfection: Follow the manufacturer’s instructions for manual or automated cleaning processes. All organic material must be removed before sterilization.
- Regular Inspection: Trained personnel in the sterile processing department (SPD) should meticulously inspect each grasper before and after sterilization. They look for:
- Bent tips or shafts.
- Cracks or corrosion, especially in hinges and insulated areas.
- Dullness of serrations or jaw misalignment.
- Proper functioning of rotation and grasping mechanisms.
- Proper Sterilization: Ensure instruments are sterilized according to validated protocols (e.g., steam sterilization/autoclaving).
- Appropriate Storage: Store instruments in protective trays or containers to prevent damage during transport and storage.
- Professional Servicing: Schedule regular professional servicing by qualified technicians to repair, sharpen, and realign instruments. This preventative maintenance is crucial for sustaining the precision and functionality of Laparoscopic Graspers.
Laparoscopic Grasper Comparison Chart (Conceptual)
To aid in the crucial process of selecting the right Laparoscopic Graspers for various surgical needs, a comprehensive comparison chart can be incredibly valuable for surgical teams. While we cannot create a dynamic, real-time table here, such a chart would typically involve the following key columns to guide informed decision-making:
| Grasper Type | Key Features (Jaw Design, Fenestration) | Primary Use | Advantages | Considerations |
|---|---|---|---|---|
| Maryland Dissector | Curved, blunt tip, fine serrations, often monopolar compatible | Blunt/sharp dissection, creating planes, cautery | Versatile, precise for separating tissues | Can be traumatic if not used carefully for grasping |
| Babcock Grasper | Broad, fenestrated jaws, atraumatic, circular shape | Holding delicate tubular structures (bowel, appendix, fallopian tube) | Minimizes crushing injury, gentle retraction | Not suitable for dense tissue, limited dissection |
| DeBakey Grasper | Long, fine, non-fenestrated longitudinal serrations, atraumatic | Gentle grasping of vessels, bowel, and fine tissue handling | Excellent for delicate tissue, less crushing | Can be slippery if wet, limited traction on dense tissue |
| Alligator Forceps | Fine, sharp teeth, strong grip | Securely grasping small, dense structures, needle retrieval | Very firm grip, good for fibrous tissue | Highly traumatic, never for delicate structures, high risk of injury |
| Kelly/Crile Forceps | Straight/curved jaws, horizontal serrations, non-fenestrated | General grasping, clamping small vessels, and passing sutures | Versatile, strong grip | Can crush delicate tissue if used improperly |
| Right-Angle Dissector | Right-angle bend at tip, fine, blunt/serrated jaw | Dissection around structures, vessel ligation in tight spaces | Access to difficult angles, precise isolation | Limited grasping ability, primarily a dissecting tool |
Laparoscopic Graspers are far more than just tools; they are the direct extension of a surgeon’s skill and intent in the complex, minimally invasive surgical field. Achieving mastery with these instruments is a continuous journey that demands a deep understanding of their various types, meticulous attention to detail in their handling, and unwavering commitment to safety protocols.
By diligently applying proven tips for instrument selection, ergonomic control, visualization strategies, and force application, surgeons can master precision laparoscopic graspers. Furthermore, a steadfast adherence to a comprehensive safety checklist and diligent instrument care are indispensable steps to effectively avoid surgical errors. Ultimately, the dedication to perfecting the use of these vital laparoscopic instruments directly translates to enhanced surgical outcomes and improved patient well-being, solidifying the foundation for excellence in modern laparoscopic surgery.
For more information about laparoscopic graspers, feel free to contact the Lapex Surgical support team.