Table of Contents
ToggleLaparoscopic Needle Holders: The Secret to Faster Suturing (Without Compromising Safety)
In the demanding environment of laparoscopic surgery, where intricate procedures are performed through minimal incisions, every second counts, yet safety remains paramount. Suturing, a fundamental surgical skill, becomes exponentially more challenging in a 2D operative field, with limited dexterity, and without direct tactile feedback. Achieving secure and precise wound closure or tissue approximation is crucial for patient outcomes, making efficient suturing a highly valued skill.
This is where Laparoscopic Needle Holders emerge as the unsung heroes. More than just instruments, they are the surgeon’s precise extensions, designed to grasp and manipulate delicate needles within the confined abdominal space. While the “secret” to faster suturing laparoscopy might seem elusive, it lies not in magic but in a profound understanding of these instruments, coupled with refined technique and an unwavering commitment to laparoscopic suturing safety.
This comprehensive article will unravel the complexities of Laparoscopic Needle Holders, exploring their various types and, most importantly, revealing the “secrets” to enhancing your suturing speed and efficiency without compromising the surgical repair’s safety and integrity. We will provide proven tips, practical techniques, and crucial safety considerations to empower surgeons to master this vital aspect of minimally invasive surgery.
The Core of Laparoscopic Suturing: Understanding Laparoscopic Needle Holders
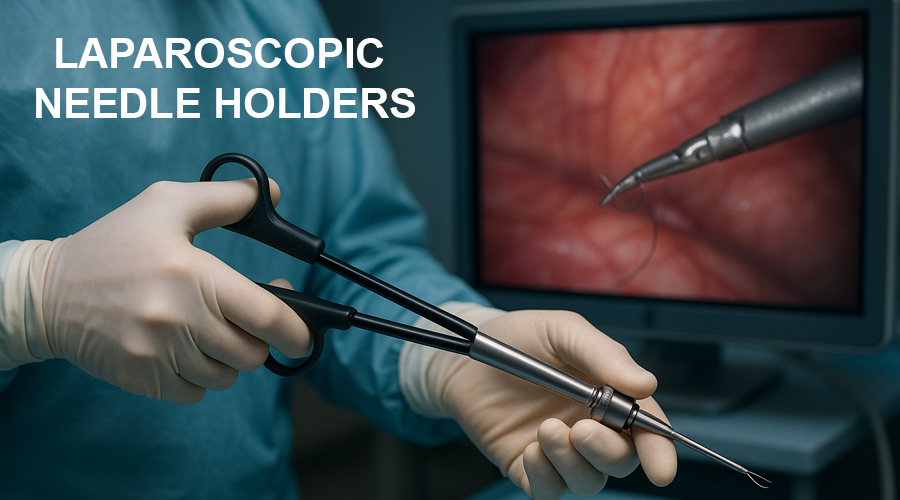
At its essence, a Laparoscopic Needle Holder is a highly specialized instrument designed to securely grasp a surgical needle, facilitate its passage through tissue, and assist in knot tying. Its mastery is central to faster suturing laparoscopic and ensuring laparoscopic suturing safety.
A typical Laparoscopic Needle Holder comprises several key components:
- The Jaws (Working End): This is the most critical part, responsible for securely gripping the needle. Jaws come in various designs (straight, curved, serrated, with or without tungsten carbide inserts) to optimize grip and control.
- The Shaft: A long, slender tube (typically 5mm or 10mm in diameter, and 30-45cm in length) that allows the instrument to reach the surgical site through the trocar. Most shafts allow for 360-degree rotation.
- The Handle: The ergonomic part held by the surgeon, designed for comfort and control. Handle types vary, affecting grip and locking mechanisms.
- The Locking Mechanism: Essential for maintaining a secure grip on the needle without continuous pressure from the surgeon’s hand. This can be a traditional ratchet or a more modern spring-loaded design.
- The Rotation Mechanism: A feature near the handle that allows the surgeon to rotate the jaws, providing an optimal angle for needle passage and knot tying.
The meticulous design of these components enables surgeons to mimic the delicate hand movements of open surgery, translating them into precise actions within the magnified, yet constrained, laparoscopic environment. A well-designed needle holder provides the tactile feedback necessary to gauge tissue resistance, crucial for both efficiency and safety.
Types of Laparoscopic Needle Holders: Matching the Tool to the Task
Just as a carpenter selects a specific hammer for a particular nail, a surgeon must choose the right Laparoscopic Needle Holder for the precise task at hand. This informed selection is the first “secret” to both faster suturing laparoscopic and paramount for laparoscopic suturing safety.
By Jaw Design
The working end of the needle holder is paramount to its function and dictates its optimal use.
- Straight Jaws:
- Description: The most common and versatile design, with jaws that align directly with the shaft of the instrument.
- Use: General purpose suturing. They provide a direct, intuitive feel and are excellent for straight-on needle passes. Most surgeons begin learning with straight jaws.
- Curved Jaws (Left or Right):
- Description: The jaws are angled approximately 45 degrees to the left or right of the shaft.
- Use: Invaluable for suturing in confined spaces or at awkward angles, such as deep in the pelvis, behind organs, or during specific anastomoses. The curvature allows for easier needle capture and passage without excessive instrument manipulation or torquing of the wrist. While they can initially feel less intuitive, mastering curved jaws can significantly contribute to faster suturing laparoscopy in challenging anatomical regions by improving “flow” and reducing fumbling.
- Tungsten Carbide (TC) Inserts:
- Description: Many high-quality needle holders feature small, extremely hard tungsten carbide inserts on the inner surface of the jaws. These inserts are often gold-handled to indicate their presence.
- Why It Works (Advantages):
- Superior Grip: TC provides an incredibly firm, non-slip grip on the needle, preventing rotation or slippage during passage through dense tissue. This direct control is vital for laparoscopic suturing safety by preventing uncontrolled needle movements.
- Enhanced Durability: Tungsten carbide is far harder and more wear-resistant than stainless steel, significantly extending the lifespan of the instrument’s jaws, even after repeated use and sterilization. This ensures consistent performance.
- Reduced Needle Damage: While providing a firm grip, the precise manufacturing of TC inserts is designed to minimize damage to the needle’s surface, preserving its sharpness for subsequent passes.
- Impact: TC inserts are a critical factor in both faster suturing laparoscopic (fewer slippages mean fewer re-grips) and laparoscopic suturing safety (predictable needle control).
- Serrated vs. Smooth Jaws:
- Most needle holders have fine serrations or cross-hatches on their jaws to enhance grip. Some specific designs might offer smoother surfaces for particular applications, though robust needle grip is generally preferred.
By Handle/Locking Mechanism
The handle design influences comfort, control, and efficiency.
- Ratchet (Finger Ring) Handle:
- Description: The traditional scissor-like handle with a locking ratchet mechanism. Once the needle is gripped, the ratchet engages to hold it securely without constant finger pressure.
- Use: Provides a very secure hold. Requires a deliberate action (often squeezing the rings further apart or using a thumb release) to disengage the ratchet. Some surgeons prefer this for its reliable lock.
- Spring-Loaded / Self-Righting Handle (Squeeze-and-Release):
- Description: These handles operate on a spring mechanism; squeezing closes the jaws, and releasing opens them. There is no traditional ratchet lock.
- Use: Favored by many for faster suturing, laparoscopic due to their quick, intuitive release. They allow for a more continuous “flow” during suturing, as the surgeon doesn’t have to consciously disengage a ratchet for each needle pass. However, they require constant finger pressure to maintain the grip, which can lead to fatigue over long cases. Some designs have a subtle internal mechanism to provide a secure, yet releasable, grip.
- Pistol Grip Handle:
- Description: A handle shaped like a pistol grip, offering a different ergonomic feel.
- Use: Some surgeons find this grip more comfortable and less fatiguing for certain movements, especially those involving pronation/supination.
By Length & Diameter
- Length: Laparoscopic Needle Holders come in various lengths (e.g., 30cm, 33cm, 45cm). Longer instruments are used for bariatric surgery or procedures in patients with a higher BMI or deep pelvic/abdominal work.
- Diameter: Typically 5mm or 10mm to match the trocar size. 5mm instruments are preferred for smaller incisions but can sometimes be less rigid, while 10mm instruments offer greater rigidity but require a larger port.
The selection of a Laparoscopic Needle Holder is not a trivial matter. It directly impacts your ability to achieve faster suturing laparoscopic and maintain laparoscopic suturing safety. A thorough understanding of these types allows surgeons to build an instrument set optimized for their specific procedures and personal ergonomic preferences.
The “Secret” to Faster Suturing Laparoscopic: Proven Techniques
Achieving speed in laparoscopic suturing is not about rushing; it’s about efficiency, precision, and minimizing wasted movements. Here are proven techniques that constitute the “secret” to faster suturing laparoscopy without ever compromising laparoscopic suturing safety.
Needle Selection & Precise Loading:
- Choose Wisely: Select the smallest needle necessary for the tissue, with an appropriate curvature (e.g., 5/8 or 1/2 circle) for the depth and angle of the bite. A needle that’s too large or too straight will be harder to maneuver.
- Optimal Loading: Grasp the needle with your Laparoscopic Needle Holder at approximately 1/3 to 2/3 of its length from the tip. This provides the best leverage for pushing the needle through tissue without bending it.
- Correct Orientation: Always load the needle in the holder so that its curvature facilitates the desired path through the tissue. Anticipate your next move and load the needle for that specific trajectory.
Ergonomics & Surgeon Comfort:
- Fatigue is the enemy of speed and precision. Ensure the operating table height, monitor position, and surgeon’s posture are optimally configured.
- Neutral Wrist: Strive to maintain a neutral wrist position to reduce strain and allow for fine motor control.
- Arm Support: Utilize armrests if available to support your forearms and minimize shoulder fatigue.
- Instrument Choice: Experiment with different Laparoscopic Needle Holders handles (ratchet, spring-loaded, pistol grip) to find what offers you the most comfort and control over prolonged periods.
The Two-Handed Approach: The “Push-Pull” Technique:
- Laparoscopic suturing is fundamentally a two-instrument skill.
- Needle Holder (Dominant Hand): Primarily pushes the needle through tissue and initiates the arc.
- Auxiliary Grasper (Non-Dominant Hand): Crucially provides counter-traction to stabilize the tissue, expose the bite, and gently guide the needle out after it exits the tissue. It can also “milk” the suture through the tissue.
- “Push-Pull”: After the needle exits the first tissue edge, instead of pushing it further with the needle holder, use the auxiliary grasper to pull the needle through, often by grasping it on its curvature. This minimizes the risk of bending the needle or stripping the tungsten carbide inserts on the needle holder. This coordinated push-pull is a cornerstone of faster suturing laparoscopy.
Mastering Depth Perception (2D Vision Aids):
- Without tactile feedback, visual cues are paramount.
- Triangulation: Position your instruments and camera to form a “working triangle” with the target tissue. This provides visual depth cues and optimal angles for instrument manipulation (ideally instruments entering at 60-degree angles to each other).
- Focusing: Use the camera’s focus to highlight the depth of the needle tip.
- Movement Feedback: Observe the interaction of the needle tip with tissue – the subtle dimpling or pushing provides visual feedback on its depth.
Efficient Knot Tying Techniques:
- Extracorporeal Knot Tying:
- Mechanism: The knot is tied outside the body using a knot pusher and then advanced through a trocar.
- Speed: Generally considered faster for beginners or quick closure of individual ports, as the knotting is done with direct hand manipulation.
- Limitations: Can be bulky, less precise for deep or difficult angles, and the knot tension might not always be perfectly controlled once it’s inside the body.
- Intracorporeal Knot Tying:
- Mechanism: The entire knot (throwing loops, grasping, pulling) is done inside the body using two Laparoscopic Needle Holders (or one needle holder and a grasper).
- Speed & Precision: While initially more challenging and time-consuming to learn, mastery of intracorporeal knot tying is the true “secret” to faster suturing laparoscopy for complex repairs (e.g., anastomoses). It offers unparalleled precision, tension control, and versatility in any surgical field. Practice involves consistent, minimal movements to form loops, grasp the suture, and tighten knots (e.g., the “C” and “S” throws for square knots).
- Automated Suturing Devices: For high-volume, long closures or specific anastomoses, automated devices (often disposable cartridges) can offer significant speed advantages. While not using traditional needle holders, they represent a technological approach to faster suturing in laparoscopy.
- Extracorporeal Knot Tying:
Suture Management:
- Organized Suture: Keep your suture material organized and free of tangles. Avoid excessive lengths of suture, as they can become unmanageable in the confined space.
- Controlled Pull-Through: After each needle pass, pull just enough suture through to allow for knot tying, avoiding excessive pulling, which wastes time and risks tangles.
- Running vs. Interrupted: For long tissue approximations, a continuous (running) suture is often significantly faster than multiple interrupted sutures. Master both for different applications.
Practice with Purpose & Deliberate Repetition:
- The journey to master precision laparoscopic needle holders for faster suturing is paved with consistent, focused practice.
- Box Trainers: Excellent for developing fundamental hand-eye coordination, needle loading, and basic knot tying.
- Virtual Reality (VR) Simulators: Offer a more realistic and immersive experience, providing performance metrics and challenging scenarios.
- Animal Labs/Cadaver Courses: Provide invaluable experience with realistic tissue handling and the tactile nuances (even if diminished through instruments) that simulators cannot fully replicate.
- Focus on efficient movements, minimizing instrument clashing, and reducing the total number of actions per stitch.
Ensuring Laparoscopic Suturing Safety: Avoiding Complications
Speed in surgery is valuable only when it does not compromise safety. Laparoscopic suturing safety is paramount, and applying the following principles is critical to avoid surgical errors related to needle and suture handling.
- Absolute Tissue Identification: Before every needle pass, unequivocally identify the tissue you are about to suture. Misidentifying bowel, a major vessel, or a nerve and inadvertently passing a needle through it is a catastrophic surgical error. Use graspers to retract, dissect, and confirm anatomical landmarks.
- Controlled Needle Passage:
- Visualize the Tip: Always maintain continuous visualization of the needle tip as it enters and exits tissue. Never make a “blind” pass. If the tip disappears from view, stop immediately, reposition the camera, or withdraw and re-attempt.
- Controlled Force: Apply steady, controlled force to push the needle through. Avoid excessive force, which can cause the needle to “pop through” unpredictably, potentially injuring underlying structures.
- Appropriate Bite: Take appropriate depth and width of tissue bites to ensure secure approximation without unnecessary tissue trauma or excessive tension.
- Maintain Suture Tension: After each stitch, maintain appropriate tension on the suture to prevent slack, which can lead to tangles, loose knots, or an insecure repair. However, avoid excessive tension that can tear tissue.
- Prevent Needle Scissoring: Laparoscopic Needle Holders are designed to hold needles, not to cut. Using them to cut sutures or tissue will dull and damage their jaws, especially the delicate tungsten carbide inserts, compromising their ability to grip needles securely in subsequent uses. Always use laparoscopic scissors for cutting.
- Rigorous Instrument Inspection (Pre-Case & Intra-Op):
- Before every case, meticulously inspect your Laparoscopic Needle Holders.
- Jaw Alignment: Ensure the jaws meet perfectly without any gaps when closed.
- Tungsten Carbide Integrity: Verify the TC inserts are intact, not chipped, or worn down. This is critical for needle grip.
- Locking Mechanism: Test the ratchet or spring mechanism for smooth engagement and release. A faulty lock can lead to needle slippage.
- Shaft Integrity: Check for bends, nicks, or damage to insulation if it’s an energy-compatible instrument.
- A compromised instrument can lead to frustrating delays, lost needles, and potentially dangerous surgical errors.
- Optimize Exposure: Ensure the surgical field is clear of blood, smoke, or other obstructions. Use efficient suction and irrigation as needed. Clear visualization is fundamental for laparoscopic suturing safety.
- Ergonomics and Surgeon Fatigue Management: Prolonged, awkward postures and repetitive stress can lead to surgeon fatigue, which in turn compromises precision and increases the likelihood of surgical errors. Take micro-breaks if possible, adjust your position, and ensure an ergonomic setup.
- Clear Communication: Maintain clear and concise communication with your scrub nurse and surgical assistant. Announce “needle in” or “needle out” to facilitate instrument counts and awareness of the needle’s whereabouts.
Advanced Considerations for Laparoscopic Needle Holders
The field of minimally invasive surgery is constantly evolving, with new technologies and approaches complementing the use of traditional Laparoscopic Needle Holders.
- Robotic-Assisted Suturing: Robotic surgical systems (e.g., da Vinci) have revolutionized laparoscopic suturing. They offer several advantages:
- 3D Vision: Provides enhanced depth perception, making suturing more intuitive.
- Wrists: Robotic instruments have articulating “wrists” that mimic the human wrist’s range of motion, allowing for greater dexterity and easier needle manipulation at difficult angles, often leading to significantly faster suturing laparoscopic for complex anastomoses.
- Tremor Filtration: The robot filters out physiological tremor, enhancing precision.
- While still requiring skill, robotic assistance can make complex intracorporeal suturing more accessible and efficient for many surgeons.
- 3D Vision: Provides enhanced depth perception, making suturing more intuitive.
- Automated Suturing Devices: For certain applications, such as long linear closures or rapid anastomoses (e.g., gastrointestinal anastomosis), pre-loaded or automated suturing devices can offer rapid tissue approximation. These instruments often replace traditional hand-suturing with pre-formed staples or specialized mechanisms, offering a different pathway to faster suturing in specific scenarios.
- Material Science Advancements: Ongoing research continues to improve the materials and coatings used in Laparoscopic Needle Holders, focusing on even better grip, enhanced durability, and improved biocompatibility, all contributing to better performance and laparoscopic suturing safety.
Instrument Care and Maintenance: Longevity and Performance
The precision and effectiveness of Laparoscopic Needle Holders are directly linked to meticulous care and maintenance. Proper handling, cleaning, and sterilization are crucial for ensuring the instrument’s longevity and, most importantly, its reliable performance during critical surgical moments, directly impacting laparoscopic suturing safety and the Cost-effectiveness of Laparoscopic Instruments.
- Immediate Post-Procedure Care: Do not allow blood or tissue to dry on the instrument. Wipe it down immediately after use and ideally immerse it in an enzymatic solution to prevent adherence of organic matter.
- Thorough Cleaning: Follow the manufacturer’s instructions for manual or automated cleaning. Pay particular attention to the jaws, hinge, and any serrations, ensuring all debris is removed. Use soft brushes; avoid abrasive materials that can scratch the surface or damage tungsten carbide inserts.
- Inspection is Key: After cleaning and before sterilization, rigorously inspect each Laparoscopic Needle Holder under magnification. Look for:
- Any signs of corrosion, nicks, or scratches on the shaft or jaws?
- Damage to the tungsten carbide inserts (chips, cracks, or excessive wear). A simple test is to try to hold a single strand of hair on the back of your hand; if it slips, the jaws are worn.
- Proper alignment of the jaws when closed; no light should show through.
- Smooth operation of the locking and rotation mechanisms.
- Integrity of any insulation is ensured if the instrument is energy-compatible.
- Proper Sterilization: Sterilize according to validated protocols. Ensure the ratchet mechanism (if present) is disengaged during sterilization to allow steam penetration and prevent heat expansion damage.
- Protective Storage: Store Laparoscopic Needle Holders in instrument trays with protective tips or separate compartments to prevent them from clashing with other instruments, which can cause damage to the delicate jaws.
- Regular Professional Servicing: Schedule routine maintenance and repair with a qualified surgical instrument repair service. They can replace worn tungsten carbide inserts, realign jaws, and ensure all moving parts are functioning optimally. This preventative approach saves money in the long run and prevents unexpected instrument failures.
Laparoscopic Needle Holders are more than just tools; they are the bedrock upon which efficient and safe minimally invasive suturing is built. The “secret” to faster suturing laparoscopy is not a shortcut, but a profound understanding of these instruments – their diverse types, the unique advantages of features like tungsten carbide inserts, and the subtle nuances of their manipulation.
By diligently applying proven techniques for needle loading, ergonomic handling, adept two-handed coordination, and mastering intracorporeal knot tying, surgeons can significantly enhance their speed and fluidity. Crucially, this pursuit of efficiency must never overshadow the paramount importance of laparoscopic suturing safety. Continuous vigilance, meticulous instrument inspection, precise tissue identification, and controlled needle passage are non-negotiable elements in avoiding surgical errors.
Ultimately, mastering Laparoscopic Needle Holders represents a cornerstone of surgical expertise in the modern era. It’s a skill refined through deliberate practice and an unwavering commitment to speed and safety, ultimately leading to superior patient care and surgical outcomes.
For more information, feel free to contact the Lapex Surgical support team.